Texans can pay thousands of dollars a month to ensure their family member is taken care of in a nursing home for the last few months or years of their life. Unfortunately, many San Antonio nursing homes are understaffed, which leads to the neglect of their patients. This neglect can manifest in physical ways, like bedsores, or pressure ulcers. Bedsores occur when patients have decreased blood flow to certain areas of their body, and are normally caused by prolonged pressure from sitting or lying down for a prolonged period of time. There are four bedsore stages, with stages one and two being the most common and treatable, and stages three and four being the most painful and the most dangerous. When a pressure sore goes untreated, it can cause deep wounds and increase a person’s risk of infection.
If your loved one has developed a pressure ulcer in a nursing home as a result of neglect, the San Antonio nursing home neglect lawyers at Janicek Law are here to help. Call us today at 210-366-4949 and schedule a free consultation with one of our professionals.
WARNING: This blog contains images of stage-one bedsore injuries. Viewer discretion is advised.
What Are Bed Sores?
Bedsores – also known as pressure sores, pressure ulcers, or decubitus ulcers – are wounds caused by prolonged pressure to a certain area of the body. They usually occur on the skin that covers bony areas of the body, like the skin on the heels, hips, tailbone, shoulder blades, and head. When an area of the body is exposed to constant pressure, it can decrease blood flow to the tissue in that area. This lack of blood can cause the surrounding skin and the deeper tissues underneath it to begin to die.
The primary prevention for bedsores is movement, whether that be changing positions when sitting or laying down, or by doing light exercise to promote blood circulation. However, some people may not have the ability to move on their own or may not even recognize that they’ve been sitting in one place for too long. That’s why they often occur in patients living in nursing homes.
It’s important for nursing homes and assisted living facilities to ensure their patients change positions, exercise, and eat healthy so pressure sores can be prevented. While not all bedsore injuries are preventable, bedsore stages three and four are almost completely preventable. When nursing home staff fail to detect or properly treat these ulcers, they may be found liable for any damages caused.
If you’re loved one suffered bed sores at a nursing care or assisted living facility, contact a San Antonio assisted living facility abuse lawyer.
What Causes Bed Sores?
Certain risk factors can increase the likelihood of someone experiencing bed sores. Those who have a lack of sensory perception due to a spinal cord injury may not feel sore after staying in one position for an extended period of time. This could cause them to develop bedsores without even realizing it. Healthcare professionals should be checking them for bedsores regularly so they can have their bedsores diagnosed and treated early.
Those who are incontinent are also prone to developing pressure sores and subsequent infections, due to their skin’s prolonged exposure to human waste. They may require additional wound care to keep their skin clean and prevent infections.
Patients with mobility issues are at high risk for developing bedsores due to their inability to change positions. Elderly care professionals must help them change their sitting or laying positions regularly in order to remove pressure from parts of their body and prevent bedsores.
Some medical devices can cause a person to experience pressure ulcers wherever the device is resting. For example, those undergoing oxygen therapy have tubing that goes over both of their ears and connects to their nose. They may not have their tubing moved often, which can cause them to develop pressure injuries on the top part of their ear.
Certain medical conditions can affect blood flow and increase a person’s risk of developing pressure ulcers. Additionally, healthy eating habits can help increase circulation and promote healthy skin, so those without proper nutrition may also have an increased risk of developing pressure sores.

What Helps Prevent Bedsores?
Pressure ulcers can be prevented in multiple ways. The primary prevention for pressure sores is by removing pressure from bony areas of the body. Moving positions frequently and participating in light exercise can promote blood flow and prevent ulcers from forming.
This helps relieve pressure on areas of the body that are prone to pressure ulcers.
Doctors often recommend patients with mobility issues use foam pads on their mattress and/or wheelchair to protect bony areas of the body from developing pressure sores. These areas include the head, shoulder blades, hips, tailbone, and heels.
Those at risk for developing a pressure injury should check their skin regularly for any change in skin color or increase in soreness. This can help detect pressure sores before they progress and cause deep tissue damage. Those at risk should also keep their skin clean and dry, and change their bedsheets and undergarments frequently.
A healthy diet can also aid in preventing bedsores and promote wound healing. Those with poor nutrition may be at a higher risk for pressure injuries.
Pressure Ulcer Stages
There are four bedsore stages, with stage one being the most mild, and stage four being the most severe. It’s important for those at risk of developing pressure sores to know the warning signs so they can prevent sores and promote healing. Below are the symptoms for the different pressure sore stages, as well as the treatments often used during the healing process.
Stage 1 Pressure Ulcer
A stage 1 pressure injury is often mild and easily treatable. In this stage, the patient won’t have an open wound.
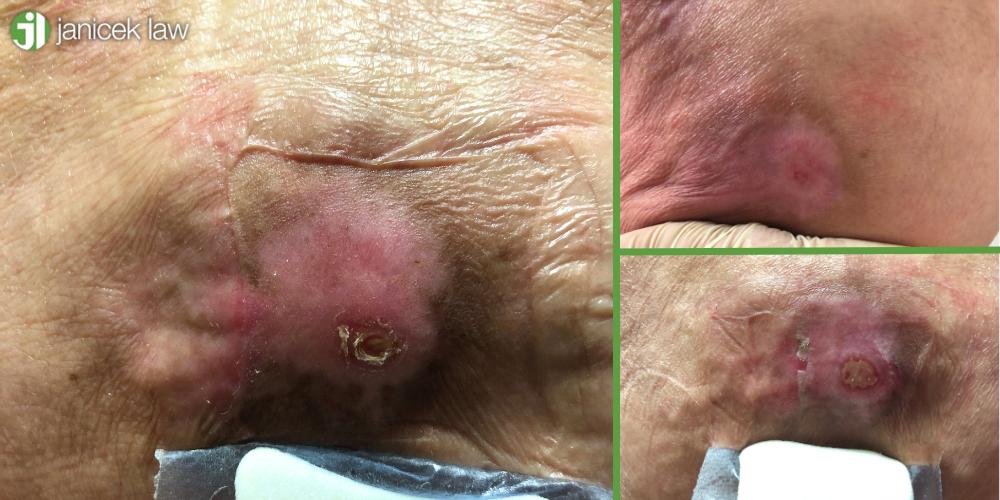
Stage 1 Bed Sore Symptoms
Symptoms of a stage 1 pressure sore include light burning or itching on and around the affected skin. The area may also feel warmer than other areas of the body and may be sore to the touch. The area can also appear discolored: patients with fairer skin will likely see redness, whereas patients with darker skin may see a bluish or purple tint in the area.
Stage 1 Pressure Ulcer Treatment
When treating stage one pressure ulcers, the first thing to do is to remove pressure from the area. This can include adding padding to the patient’s mattress or wheelchair, or ensuring the patient changes position frequently.
Keeping the ulcer clean and dry can also help prevent it from progressing to a later stage. Stage one ulcers can heal in about three days from onset of symptoms.
Stage 2 Pressure Ulcer
Stage two pressure ulcers are often more visible and painful than stage one pressure ulcers. In stage two bedsores, the skin breaks open, creating an open wound. These are the most common types of bedsores found in nursing homes and can be easy to diagnose.
Stage 2 Bed Sore Symptoms
Stage two decubitus ulcers often create a crater in the skin. Some patients may develop a blister in the area. The ulcer may have drainage and leak clear fluid, and it may be more painful and sore than it was before.
Stage 2 Pressure Ulcer Treatment
Stage two pressure sores can also be treated by removing pressure from the affected area. Since stage two pressure sores are open wounds, proper skin care can help promote healing. Healthcare professionals may clean the area with mild soap and water, and apply dressings to protect it from germs and debris. They may also apply moisture barrier creams to the skin surface to help the body dissolve any dead tissue, which can prevent the skin from flaking and sloughing off.
Stage 3 Pressure Ulcer
At stage three, the pressure sore will have broken through the first two layers of skin and may begin affecting the deeper tissues. Stage three pressure ulcers should be inspected for any signs of infection so that it can be treated as soon as possible.
Stage 3 Bedsore Symptoms
Stage three pressure sores will look like a hole or crater in the skin. The skin breakdown may reveal the fatty tissue beneath the skin. The decubitus ulcer may be infected if it is leaking pus or discolored drainage, or if it is emitting a foul odor.
Stage 3 Pressure Ulcer Treatment
Stage three pressure sores require immediate medical treatment. A doctor may remove dead tissue from the wound or surrounding area to promote healing, and may prescribe antibiotics to treat an infected bedsore.
Stage 4 Pressure Ulcer
Stage four pressure ulcers are the most serious. Pressure injuries that have progressed this far may have reached into the underlying tissue, like muscle, ligament, or even bone. Stage four pressure ulcers have a higher risk of infection than ulcers at other stages.
Stage 4 Besore Life Expectancy and Symptoms
At stage four, decubitus ulcers will appear as a deep, open wound, and, depending on the depth of the ulcer, the patient’s muscle or bone may be visible at the bottom of the crater. The wound may also be exhibiting signs of infection, like drainage or foul odor.
Stage 4 Pressure Ulcer Treatment
A stage four pressure ulcer requires immediate medical treatment. In addition to keeping the area clean, dry, and properly dressed, doctors may have to perform surgery to remove any dead tissue from the site of the ulcer.

What Causes Bedsores in Nursing Homes in Texas?
Pressure ulcers can be a sign of nursing home abuse and neglect. If nursing home staff aren’t properly preventing and treating pressure sores, they may be found negligent in an elder abuse case.
Nursing homes with a small staff are often unable to give every patient in their care the amount of time and attention they need to stay healthy. Understaffed nursing homes can cause elderly patients to experience prolonged pressure on parts of their body where pressure ulcers are common, since there are fewer people there to move and reposition the patients. Pressure injuries may also go completely unnoticed, which can cause them to progress to a later, more painful stage.
An untreated decubitus ulcer can cause serious health problems and can even lead to death. If you or your loved one has developed a pressure sore in a nursing home, you may be able to recover financial compensation for damages. Call the San Antonio nursing home death attorneys at Janicek Law today at 210-366-4949 and schedule your free consultation to discuss a potential elder abuse claim.
Risk of Having Bedsores
Developing bedsores can put a person’s life at risk. When bedsores begin to make their way into the later stages, they put the person suffering from the pressure sore at a higher risk of developing an infection. If the infection spreads outside of the affected area, it can lead to additional health complications, like bone infections, joint infections (also known as septic arthritis), and blood infections.
Can You Sue a Nursing Home For Bed Sores in Texas?
Yes, if you develop a pressure sore in a nursing home, you may be able to sue the nursing home or assisted living facility for damages caused. Nursing home staff should be taking steps to help relieve pressure in ulcer-prone areas and should be inspecting their patients regularly for the warning signs of pressure ulcers. When staff fail to take these steps, they can cause patients to develop painful and even life-threatening medical conditions as a result.
Nursing home staff should not wait until their patient begins showing signs of infection before treating decubitus ulcers. If you or your loved one has suffered from a pressure sore as a result of nursing home neglect, call Janicek Law at 210-366-4949 to speak with an experienced San Antonio nursing home bedsore lawyer.
Nursing Home Abuse and Neglect Damages
Damages from nursing home injuries, like a suspected deep tissue injury, vary from case to case. When the elderly develop severe pressure ulcers as a result of neglect, they can recover compensation for things like medical bills, physical pain and suffering, and emotional distress. If a patient dies as a result of a pressure ulcer, their family can recover compensation for funeral expenses and burial costs.

San Antonio Bedsore Lawyers
Decubitus sores are treatable and, in many cases, avoidable. Despite this, many nursing homes across the country fail to check for the warning signs and properly treat pressure sores before they progress. This can leave their patients in pain and at risk for life-threatening health conditions as a result. If you or your loved one has developed a pressure sore due to negligence, call Janicek Law today. With over 20 years of experience, you can rest assured that your elderly abuse case is in good hands. Call us today at 210-366-4949 to discuss your case with a San Antonio nursing home abuse and neglect lawyer.

